If you’ve ever experienced an intense, frequent, and urgent need to pee, but when you reach the bathroom, you barely squeeze out a drop—and man does it burn!—you’re certainly not alone.
Most often these symptoms indicate a urinary tract infection (UTI). As one of the most common types of infection, 50-60% of women have at least one UTI in their lifetime. Men also get UTIs, although they’re less common for them. For every eight women who get a UTI, one man will get one.
To add some confusion, there are different types of UTIs. The names of these infections are determined by which part of your urinary tract is infected. Types of UTIs include bladder infections, kidney infections, and urethra infections.
Whatever type of UTI you have, prompt diagnosis and treatment (typically in the form of antibiotics) will usually get rid of it and the symptoms within two or three days. To help speed recovery and reduce the chance of complications, this article will explain the different types of UTIs, their varying symptoms, and options for treatment.
What Is a Urinary Tract Infection?
First, an anatomy lesson: The urinary tract contains the urethra, bladder, ureters, and kidneys. All of these organs work together as our body’s drainage system, making and removing urine, which carries waste and extra fluid from our body.
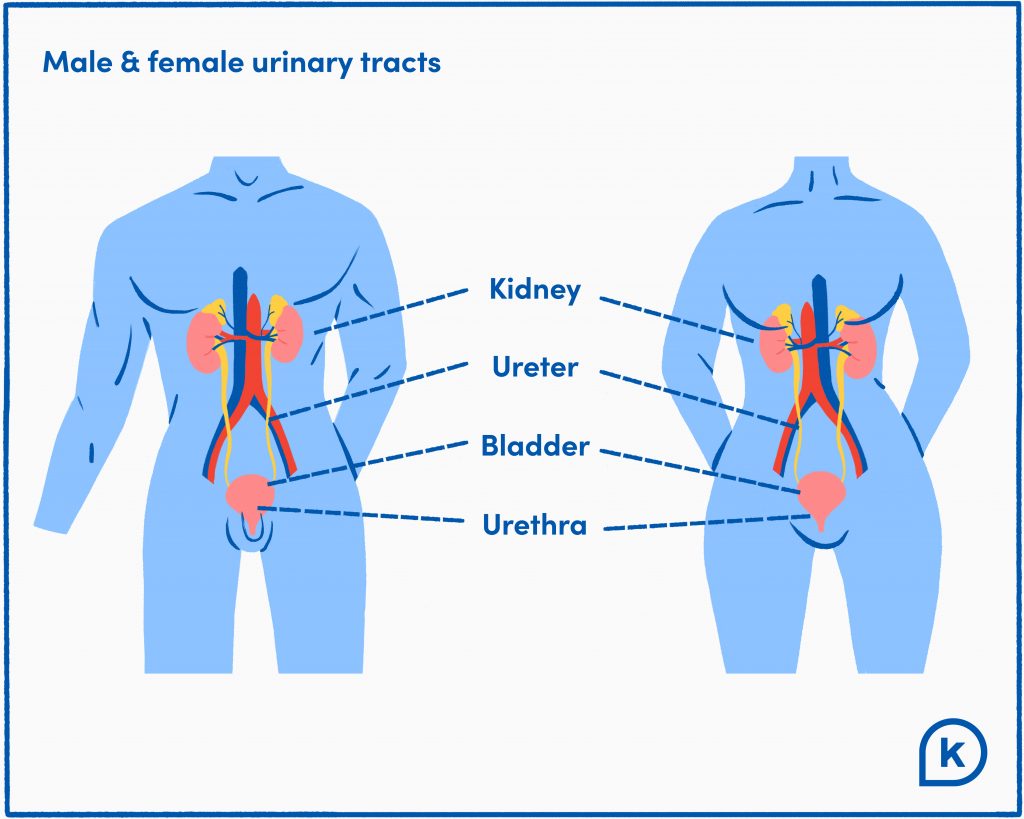
A urinary tract infection is an infection that occurs in any part of the urinary tract. Most UTIs occur in the lower urinary tract (the bladder and the urethra), though they can spread to the upper urinary tract (the kidneys). UTIs that target and stay in the lower urinary tract are referred to as simple UTIs.
No matter where a urinary tract infection occurs, UTIs can create severe discomfort or pain, especially when urinating.
Types of UTIs
The type of UTI you have depends on where in your urinary system the bacteria have attached themselves and reproduced. The three types of UTIs are:
- Bladder infection (Also called cystitis)
- Kidney infection (Also called pyelonephritis)
- Urethra infection (Also called urethritis)
Missing from this list are the ureters. These are the tubes that carry urine from the kidneys to the bladder. While ureters are rarely infected, they can transfer infectious bacteria from one organ to the other within the urinary tract. If bacteria spreads within our urinary system, it can lead to multiple UTIs and potential health complications.
For instance, an untreated bladder infection could lead to a more serious kidney infection. And an untreated kidney infection could lead to long-term kidney damage or even to an infection outside of the urinary tract. This is why prompt UTI diagnosis and treatment are important–to prevent or stop the spread of bacteria.
As we’ll discuss, each type of UTI has its own causes, symptoms and risks, though many may overlap. This makes it hard to differentiate between them, which is why your doctor may refer to your infection as a general UTI instead of a more specific type.
Either way, it’s best to seek medical attention at the first sign of any urinary discomfort. Your doctor will most likely treat you with UTI medicine, specifically antibiotics, which usually take effect within 2-3 days.
What Causes a UTI?
In general, UTIs are caused by bacteria that enter the body through the urethra and then multiply in an area or areas of the urinary tract.
Escherichia coli (E. coli) are overwhelmingly the most common cause of bladder and urethra infections. An estimated 80-90% of UTIs are caused by this bacteria. UTIs can also be caused by:
- Fungi: Though rare, fungi can infect the urinary tract.
- Genetics: Abnormalities in the shape of your urinary tract or simply inheriting certain genes can make you more likely to get UTIs.
- Other bacteria: Other bacteria, such as staphylococcus infections, can cause infections through the urethra and sometimes even infect the kidneys from the bloodstream.
- Infected prostate: A prostate infection may cause a UTI in men because an enlarged prostate makes it harder to fully empty the bladder.
What causes UTIs in women may differ from men thanks to women’s physiology. First, a woman’s urethra is shorter than a man’s. Second, the opening of a woman’s urethra is close to the vaginal opening and the anus.
Both of these factors make the path shorter and faster for bacteria to travel from the vagina or anus (after sexual activity or a bowel movement) to and then through the urethra to the bladder. From the bladder, the infection can spread through the ureters to the kidneys if it’s left untreated.
UTI Symptoms
Most UTI symptoms involve urination. However, there are other symptoms that affect your mid-section. Additionally, although many of the symptoms of UTI in women also occur in men and older adults, each of these groups also has some unique symptoms.
Depending on the type of UTI you have, its severity, your sex, and your age, you may experience one, many, or none of the following symptoms:
- An intense, persistent and frequent urge to urinate
- A burning sensation or pain when urinating
- Passing frequent, small amounts of urine
- Cloud-colored urine
- Blood in the urine
- Strong or foul-smelling urine
- Pelvic pain (UTI symptom for women only)
- Pain in the side, lower abdomen, or back
- Nausea and/or vomiting
- Fever
Additional UTI Symptoms in the Elderly:
- Pain in the lower abdomen or back
- Chills
- Constipation
- Urinary incontinence
- Sudden, new confusion or delirium
Lastly, each type of UTI may have more specific signs and symptoms. Here are the most common signs and symptoms according to the following UTIs:
Bladder infection (cystitis)
- Pelvic pressure
- Muscle aches and/or discomfort in the lower abdomen
- Frequent, painful urination
- Blood in urine
Kidney infection (pyelonephritis)
- Upper back and side pain
- High fever
- Chills and/or shaking
- Nausea
- Vomiting
- Symptoms of a bladder infection may also be present at the same time
As you can see, since some of the symptoms may overlap, it can be difficult to determine which part of your urinary tract is infected. It can also be easy to mistake the symptoms for another type of ailment. That’s why it’s best to visit your doctor for a professional diagnosis at the first sign of urinary discomfort.
How Is a UTI Diagnosed?
In order to diagnose and prescribe the best antibiotics to treat a UTI, doctors start by asking about your symptoms and any history of UTIs. Then, oftentimes, they will do a physical exam to check for tenderness in your pelvis, back, and sides.
The next step is to test your urine with a urine sample and/or a urine culture. These urine tests help determine whether you have a UTI and what type of bacteria is causing the infection. This diagnosis will help figure out what type of treatment will be most effective. After all, some bacteria are resistant to certain types of antibiotics.
If you experience frequent UTIs, your doctor may advise doing an imaging study of your urinary tract. The following tests can help determine if there is an abnormality in your urinary tract:
- Ultrasound of the kidneys and bladder
- CT scan or MRI of the urinary tract
- Cystoscopy: This is when your doctor inserts a tube-like instrument with a lens into your urethra and bladder for an internal exam.
For a male UTI, if the doctor suspects you may have an enlarged prostate gland, they may also perform a rectal examination. While wearing gloves, the doctor inserts a lubricated finger into the anus to feel the prostate gland and check for any bumps or other abnormalities.
UTI Risk Factors
Anyone—male or female, young or old, sexually active or not—can get a UTI. At the same time, certain risk factors that increase the likelihood of developing a UTI. These include:
- Sex. Women are 30 times more likely to get a UTI compared to men. This is due to women’s physiology. Their shorter urethra and the proximity of the opening of the urethra to the vaginal opening and the anus makes it easier for bacteria to travel into the urinary tract.
- Age. Older adults are more susceptible to UTIs because they are more likely to have difficulties emptying their bladders. The risk is particularly higher for those 85 and older.
- Diabetes. Especially if uncontrolled, this condition can weaken the body’s immune system to fight off infection.
- Sexual activity. Any sexual activity can cause bacteria in the urinary tract, which can potentially lead to infection. Having sex more frequently or with multiple partners may also increase the risk of UTI.
- Spinal cord injuries: People with such an injury have an average of 2.5 UTIs each year. A spinal cord injury or other nerve damage can make it difficult to empty your bladder regularly and completely.
- Menopause: The prevalence of UTI in women 65 and older is about double that of all women. This is the age when menopause sets in. This may cause changes in the bacteria that live inside a woman’s vagina.
- Urinary catheters: When this tube is placed in the urethra and bladder to drain urine, it can introduce bacteria into the urinary tract.
- Bowel incontinence: People with bowel incontinence are three times more likely to develop a UTI.
- Urinary tract blockage: The presence of kidney stones, a tumor, an enlarged prostate, or any other condition can block the flow of urine.
- Recent urinary tract procedures: Surgery or a urinary tract exam that involves medical instruments can increase the risk of developing an infection.
- Certain forms of birth control: Spermicides or unlubricated condoms may cause skin irritations that allow bacteria to invade.
- Antibiotics: Although antibiotics are often the first-line treatment for UTIs, they can also affect the balance of the natural microflora in your urinary tract. Sometimes this can actually lead to UTIs.
UTI and Pregnancy
About 8% of pregnant women will experience a UTI while expecting. As the uterus expands, it puts pressure on the bladder. This can make it more difficult to empty your bladder and, in turn, increase the risk of bacteria growing there. Plus, the increase in progesterone that causes muscles to relax also causes the urethra to expand, making it much easier for bacteria to crawl inside.
The symptoms of UTI in pregnant women are the same as in any woman, however, some expecting mothers have asymptomatic bacteriuria. A urinalysis finds bacteria in their urine, yet they don’t experience any symptoms.
In either case, doctors typically treat the UTI or asymptomatic bacteriuria with an antibiotic because both post a higher risk of UTI-related complications, like developing a kidney infection. Hormonal and anatomic changes make it easier for bacteria to spread from the bladder through the ureters to the kidneys. A kidney infection during pregnancy can lead to serious infections in the mother as well as early labor and low birth weight in infants.
Chronic UTIs
Chronic or recurring UTI is when someone has three or more UTIs in a year or two or more UTIs in six months.
Just as with any UTI, chronic UTI is more common in women than in men. In a study of college women who had a first UTI, about a quarter got another UTI within six months and almost 3% had a third UTI in that time. In another study, more than half of women 55 and older reported another UTI in the next year.
Many of the same risk factors for UTIs in general make people more prone to chronic UTI. These risks are most common in the following people:
In premenopausal women:
In postmenopausal women:
- Changes in estrogen levels cause changes in the microbiome of the vagina.
- Increased risk of incontinence and difficulty in completely emptying the bladder during urination.
In men:
- Enlarged prostate can make it harder to properly empty the bladder. And any collection of urine like that is an attractive place for bacteria to grow.
UTI Treatment Options
Although the main treatment for UTIs is antibiotics, some home remedies may also help. Additionally, sometimes doctors will prescribe other medications along with the antibiotics. Below are the most common treatment options.
Antibiotics for UTI
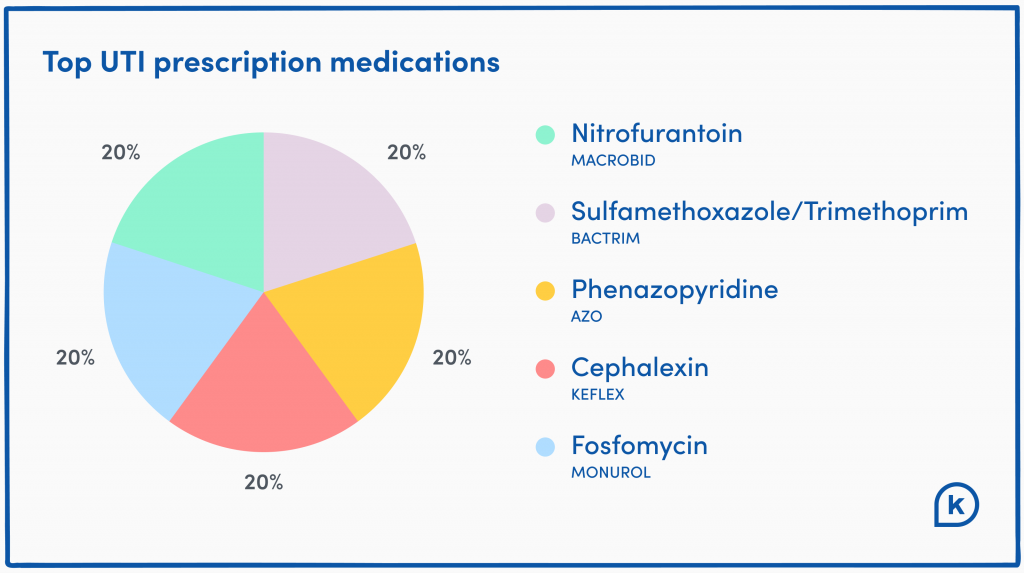
Antibiotics are usually the first—and most recommended—course of treatment for UTIs. Doctors use the results of a urine culture to identify which bacteria are causing the UTI. Then they can prescribe the best type and dosage of antibiotics to get rid of that bacteria and the infection.
The UTI antibiotics used vary based on if you have a simple UTI, severe UTI, or chronic UTIs.
Learn: Antibiotics for UTI: What’re Your Options?
Treatment for a simple UTI
Simple UTIs are those that occur in the urethra and bladder in the lower urinary tract.
Oral antibiotics are usually enough to treat these.
It’s important to take the entire course of antibiotics as prescribed, even if the symptoms subside after a couple of days. Your doctor may also prescribe pain medication to ease any pain or burning when urinating until the antibiotics take effect.
For UTI in elderly populations, doctors typically use narrow-spectrum antibiotics (such as amoxicillin) because these have a lower risk of antibiotic resistance and side effects.
Treatment for severe UTIs
For severe UTIs, like complications related to kidney infections, or UTIs associated with pregnancy, you may need to be treated in a hospital where you could receive intravenous antibiotics.
Treatment for chronic UTIs
If you have chronic UTIs, your doctor may recommend other kinds of treatment, such as:
- Low doses of antibiotics given for an initial six months (and sometimes longer).
- One dose of antibiotics given after sexual intercourse if your UTI is related to sexual activity.
- Vaginal estrogen therapy via a topical cream or suppositories for postmenopausal women.
Home remedy treatments for UTIs
While doctors will almost always recommend antibiotic treatment for UTIs, there are also complementary home remedies for UTI pain and discomfort relief that can help until the antibiotics kick in. These may include:
- Drinking plenty of water (and/or cranberry juice) to dilute your urine, which will help you urinate more, thereby helping to rid the urinary tract of the bacteria.
- Avoiding coffee, alcohol, and drinks that contain citrus juices or caffeine, which can all irritate your bladder and/or intensify the frequent/urgent need to urinate
- Using a warm (not hot) heating pad on your abdomen to ease bladder pressure or discomfort
Related Conditions
Most of the time, especially when treated promptly and with the full course of an appropriate antibiotic, urinary tract infections can clear up within a few days. However, if a UTI is left untreated, if treatment is delayed, or if you do not take all of the antibiotics, serious complications can develop. Such UTI complications may include:
- Long-term or permanent kidney damage: An untreated UTI can spread to the kidneys where it can develop into an acute or chronic kidney infection.
- Sepsis: Bacterial infections can sometimes lead to sepsis, where the entire body reacts by becoming inflamed. This wide-spread inflammation can be life-threatening, especially if the infection spreads from the kidneys into the bloodstream.
To reduce the risk of any complications, it’s in your best interest to see your doctor for treatment.
Preventing UTIs
Many factors can encourage bacteria to grow and spread within your urinary tract. The good news is, simple habits can help reduce the risk of future UTIs. Try to follow as many of the following tips as you can:
- Drink plenty of fluids, especially water. This will encourage you to use the bathroom more often, thereby helping to flush extra bacteria from your urinary tract.
- Urinate regularly. As much as you can, don’t hold in urine.
- Do not use douches or deodorant sprays in the genital area, as this may irritate the urethra.
- Wipe from front to back after urination and bowel movement.
- If you’re prone to recurring UTIs, try to empty your bladder shortly after sexual intercourse.
- If you are menopausal and have chronic UTIs, talk to your doctor about topical estrogen therapy.
When to See a Doctor
Since most UTIs are easily treated, it’s best to see your doctor at the very first sign of symptoms. Getting an accurate diagnosis is important to rule out any other disease, such a sexually transmitted disease, which can have similar symptoms.
Some patients may need their urine to be cultured to determine the correct antibiotics.
In addition to wanting fast relief for your symptoms, immediate treatment will help prevent any medical complications that can arise when infection spreads, namely a kidney infection.
How K Health Can Help
Did you know that you can get UTI treatment online through K Health?
We have clinicians available 24/7 to get you the care or medication that you need.
Frequently Asked Questions
K Health articles are all written and reviewed by MDs, PhDs, NPs, or PharmDs and are for informational purposes only. This information does not constitute and should not be relied on for professional medical advice. Always talk to your doctor about the risks and benefits of any treatment.

 Medically reviewed
Medically reviewed
